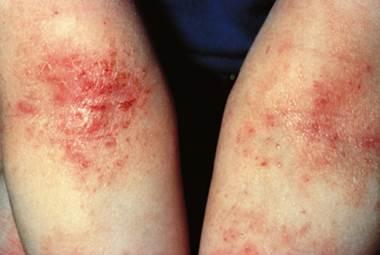
Eczema
Eczema, also known as atopic dermatitis, is a chronic skin that causes areas of red, itchy skin. This condition usually starts in early childhood, especially when there is a family history of atopy (asthma, hay fever, conjunctivitis, or food allergies). The skin fails to hold in moisture, becomes dry, then inflamed, itchy and often infected. Various combinations of factors cause the dryness. Allergies leading to an overactive immune system and hereditary dry skin (ichthyosis vulgaris) are the most prominent internal and external factors.
To treat this disease you need to work with the doctor in identifying and reducing those factors that trigger of flare-up the disease. These are different for each person, so no one therapy is appropriate for all eczema patients.
Treatment
Skin becomes dry, not because it lacks grease or oil, but because it fails to retain water. Therefore, to correct dryness, water is added to the skin, followed by a grease or oil-containing substance to hold the water in.
Soaking the affected area, in a basin, bath, or shower, for 15-20 minutes using lukewarm water, can help to hydrate the skin. Hot water dries out the skin. Avoid vigorous use of a washcloth in cleansing. When toweling dry, do not rub the skin. Blot or pat dry so there is still some moisture left on the skin, and immediately apply a moisturising cream.
Moisturising lotions contain some water, so they are not as effective. Use of moisturisers without first trapping in water is also less effective. Many patients find that two or three additional applications of moisturisers during the day give additional help.
Tar Preparations
Tars and extracts of crude coal tar are often used to reduce the amount of topical steroids needed in chronic maintenance of eczema. A pharmacist can make up one to five percent LCD (Liquor carbonis detergens) in a cream. Tar gel products (Estar Gel and Psorigel) are available, but they contain alcohol and may cause burning and irritation on already red and inflamed skin, so are not recommended.
Steroids
Topical steroids are particularly useful to treat flare-ups of eczema. They help keep down the inflammation and itching. Apply them just on the rash (instead of the oil recommended above) especially after a soak or bath. Do not use topical steroids more than twice a day.
Hydrocortisone ointment or cream can be used for eczema in infants and young children, or in skin folds in adults. More potent topical steroids should not be used on thin-skinned areas of the face, neck, armpit, and groin. Short, supervised courses of medium potency topical steroids creams are safe and effective for flares of eczema on other parts of the body. Adverse effects of long term topical steroids include thinning of the skin (atrophy), a change in the color of some skin (depigmentation), and acne-like eruptions.
A newer class of topical drugs are the 'topical immunomodulators' or TIMs. These locally calm down the immune system similar to topical steroids. However they don't have the side effect of steroids in that they do not cause thinning of the skin with long term use. There are currently two of these drugs available: Protopic (tacrolimus) Ointment and Elidel (pimecrolimus) Cream. They can be used in patients two years of age or older.
Ultraviolet Light
Ultraviolet light (UVB or PUVA) therapy may be of some help in chronic eczema that does not respond well to other therapy. UVB and PUVA require three per week and must be used under professional supervision. However, avoid sunburn and hot or humid conditions that might make your skin even itchier. The risks of UVB or PUVA are sunburn and increased risk of skin cancers if used for too long.
Antipruritics
Itching is often the most aggravating of all eczema symptoms. Antihistamines may provide some relief. The antihistamines reduce scratching mainly through tranquilising and sedative effects. It takes several weeks of use on a regular basis to help. This is because scratching aggravates the eczema, keeping it from healing. Cutting nails, and using cotton gloves at night can minimise scratching. The topical use of antihistamines such as benadryl should be avoided, because it is ineffective and may produce allergic reactions.
Corticosteroids
Oral steroids should be minimised because of the seriousness of their side effects and the potential for severe flares of eczema when they are discontinued. If these are used for severe flares, then intensified skin care will help to suppress the flaring of the eczema during a taper from oral steroids.
Immunosuppressants
These are a group of medications that reduce the activity of immune system responsible for the excessive inflammation and hence decrease the severity or clear the eczema fully. Methotrexate, azathioprine, mycophenolate mofetil, ciclosporin are the most commonly used immunosuppressants when long term systemic treatment is needed, in the most severe cases.
Eczema Infection
Flare-ups and hard to control eczema are sometimes due to a coexisting bacterial, and sometimes fungal or viral, infection. If your eczema is weeping or oozing, if it crusted, or if it has small bumps, your doctor will probably test or treat for bacterial infection.
Systemic antibiotics are often necessary to decrease the irritation caused by bacteria on the skin. Most patients with eczema have Staph bacteria on their skin, and this can cause irritation even without overt infection. In acute flares, antibiotic treatment usually lasts from 14 to 28 days. Chronic maintenance antibiotics may be used if you develop infections repeatedly. Some have found success by adding very dilute bleach to the bathwater-no more than a tablespoon for a full bathtub. Topical antibiotics are not recommended and most antibacterial cleansers may actually worsen the condition.
Rarely, the cold sore virus (Herpes simplex) may cause extensive local or widespread infection, and is usually treated with oral antiviral medication.
Xerotic & Gravitational Eczema
Xerotic eczema, also called asteatotic eczema or eczema craquelé, is a form of eczema that occurs when the skin becomes abnormally dry, itchy and cracked. It is more usually found on the legs of elderly people, though it is not uncommon for people in their twenties. It can appear as red, dry flakey patches most commonly on the lower legs as well as the thighs, chest and arms. Xerotic eczema sometimes occurs in combination with Gravitational eczema, which is associated with poor circulation. Over time, if left untreated, the skin can develop eczema, with red, itchy spots, dryness, flaking and in some cases, leg ulcers.
Seasonality is prominent, and most people develop symptoms in the winter months, especially in areas where indoor humidity is decreased by heating. This explains why the frequency during the winter season is increased. Those with this skin condition may notice symptomatic improvement in a warm, humid climate in and outdoors.
Shaving, wool, or other sources of irritation can also cause a person's dry skin to become inflamed. Controllable risk factors include: frequency of bathing, the types of soaps and cleansers used in bathing, the types of skin lubricants used, diet and medications. Risks factors for dry skin should be minimised as they interrupt the components of the outer layers of the skin. The disruption in the skin barrier can lead to eczema.
As with most conditions, prevention is key in controlling xerotic eczema. Much of the problems associated with dry skin can be helped through simple behavior changes. Short, cool showers with a mild, fragrance free soap or soaks with added bath emollients are recommended.
Try to avoid harsh skin cleansers that dry the skin even more. Within three minutes of bathing, a petroleum-based emollient such as Vaseline should be applied such as. Gentle moisturising throughout the day is also encouraged. Agents that contain urea and lactic acids are good choices. Light, non-restrictive clothing that doesn't irritate or lead to itching is also preferable.
Itching may be helped by some oatmeal baths and menthol/camphor lotion. In the home, the installation of a humidifier may also help during the winter season. In severe cases, the application of topical steroids can be used in short courses when supervised by your physician.


